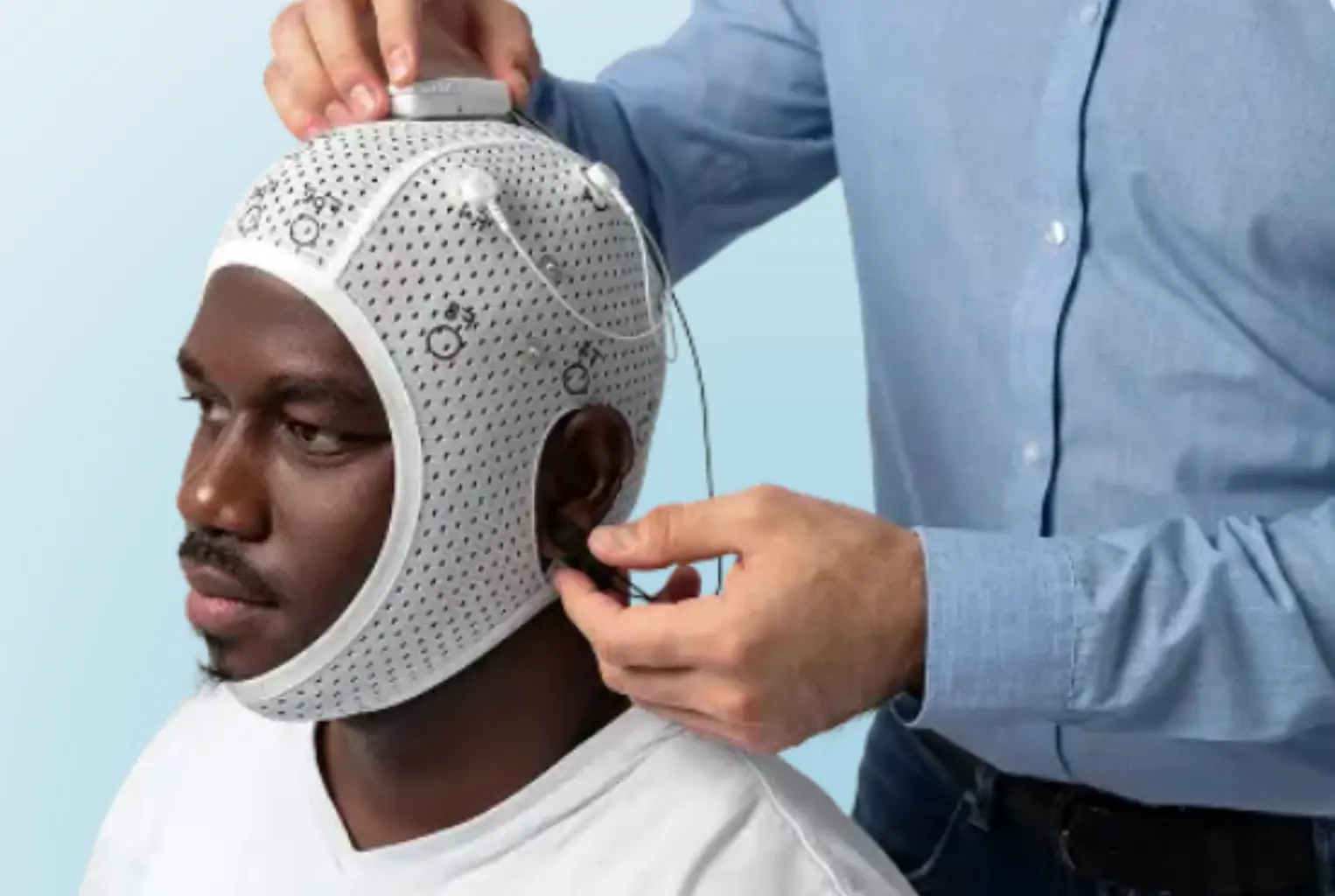
The difference between guessing and measuring
Four electrodes at Cz, Fz, F3 and F4 capture your brain’s electrical activity in real time. Seven minutes of recording, same-day report, objective data your GP can act on.
You've spent years wondering. You've taken every online quiz going. You relate to every ADHD post on social media. You're not looking for another checklist — you want to know what your brain is actually doing. We measure it.
ADHD doesn't magically disappear when you turn 18. Research shows that up to 65% of children with ADHD continue to have clinically significant symptoms into adulthood. But the majority were never diagnosed as children — especially women, and especially anyone who wasn't the "disruptive hyperactive boy" stereotype.
If you're reading this page, there's a good chance you've spent years developing coping mechanisms that mask the underlying neurology. You're not lazy. You're not stupid. You're not "just disorganised." Your brain may be wired differently — and there's a way to measure that objectively.
There's been a surge in adult ADHD awareness, partly driven by social media and partly by better clinical understanding. The Royal College of Psychiatrists now recognises adult ADHD as a widely underdiagnosed condition. Many adults are seeking assessment in their 30s, 40s, and beyond — often triggered by their child being diagnosed, by workplace struggles reaching a crisis point, or by a TikTok video that makes them think "that's me."
The problem is that the NHS pathway for adult ADHD is even more backlogged than the children's pathway. Adult ADHD assessment waiting times are typically 3-5 years in most NHS trusts. The NICE guidelines (NG87) recommend timely assessment, but the system can't deliver it. Private psychiatric assessment costs £700-£1,500. And both routes rely entirely on conversation — no objective brain measurement.
That's the gap we fill. In 30 minutes, we can measure the theta/beta ratio in your brain — the most-studied EEG biomarker for ADHD — and compare it against published norms for your age group. You walk out with objective data, not opinions.
You know what needs doing. You want to do it. You just... can't start. The deadline passes. Guilt spirals. You promise yourself next time will be different. It isn't.
Your body might be still but your mind never is. Racing thoughts. Can't switch off at night. Always needs to be doing something. Boredom feels physically painful.
You're perpetually late — not because you don't care, but because time genuinely feels different to you. An hour can feel like 10 minutes. You consistently underestimate how long things take.
You can spend 14 hours on something that interests you and forget to eat. But the boring-but-important task? Can't give it 20 minutes. It's not a motivation problem — it's a dopamine regulation problem.
Rejection sensitivity. Disproportionate reactions to minor setbacks. Quick to frustration, quick to enthusiasm. People tell you you're "too much" or "too sensitive." It's exhausting.
You've built systems, alarms, lists, and workarounds that let you function. Nobody sees the effort it takes. You appear competent on the surface but you're running on fumes. One more plate and everything crashes.
Frequent job changes. Unfinished projects. Partners frustrated by forgotten commitments. You're capable of extraordinary things — but consistency is the struggle nobody sees.
"Everyone struggles with this." "I'm just lazy." "If I tried harder..." Sound familiar? Undiagnosed adults often internalise their difficulties as personal failures rather than neurological differences.
If you recognise yourself in several of these patterns, it's worth investigating. Our brain screening measures the underlying neurological pattern — elevated theta relative to beta activity — that is associated with ADHD across all ages. It doesn't matter whether you're "obviously ADHD" or you've been masking for decades. The brain data tells the story that your coping mechanisms hide.
We place a lightweight cap with four dry electrodes on your scalp — Cz (central midline, the FDA-standard site), Fz (frontal midline), F3 (left frontal), and F4 (right frontal). No gel, no needles, no discomfort.
Phase 1 (2 minutes): Eyes open, looking at a fixation cross. We capture your resting brain state — the baseline pattern your cortex produces when alert but not task-engaged.
Phase 2 (2 minutes): Eyes closed, relaxed. Your brain shifts into a different pattern. Comparing the two conditions reveals information about cortical reactivity.
Phase 3 (3 minutes): Go/No-Go attention task. Green circle = press. Red square = don't. This measures sustained attention, impulse control, reaction time, and response variability — the cognitive functions most affected by ADHD.
We compare your results against age-matched norms. The theta/beta ratio naturally decreases with age as the brain matures, so a 25-year-old and a 50-year-old have different reference points. Our database covers age groups 18-25, 26-40, 41-60, and 60+ — all sourced from published peer-reviewed research including Arns et al. (2013) and Monastra et al. (1999).
To be clear: we don't position this as a replacement for clinical assessment. ADHD diagnosis should involve clinical interview, behavioural history, and assessment of differential diagnoses. But our screening provides the one thing no questionnaire can — a direct measurement of your brain's electrical activity, compared against published norms, with a z-score showing exactly how many standard deviations you fall from the healthy average.
The American Academy of Neurology found that accuracy reaches 89-94% when TBR data is combined with clinical evaluation. Your clinician brings the interview. We bring the brain data. Together, they paint the complete picture.
Yes. The theta/beta ratio biomarker is validated across all ages. Our normative database includes adult age groups (18-25, 26-40, 41-60, 60+). Many of our clients are adults in their 30s and 40s who have suspected ADHD for years and want objective data before pursuing formal diagnosis.
Absolutely not. We regularly screen adults in their 40s, 50s, and beyond. Brain patterns associated with ADHD don't disappear with age. If anything, a later-life screening can explain decades of struggles that were never properly understood. It's never too late for answers.
The underlying neurology is the same. But the behavioural presentation evolves. Physical hyperactivity often becomes mental restlessness. Inattention manifests as difficulty with deadlines, organisation, and sustained focus at work rather than "can't sit still in class." Our screening measures the brain pattern, not the behaviour — so it works regardless of how symptoms present outwardly.
Online quizzes measure subjective self-report — how you perceive your own behaviour. They're useful as a first indicator but they can't measure what's happening in your brain. Our screening measures actual electrical brain activity and compares it against published norms with z-scores. It's the difference between "I think I might have ADHD" and "my theta/beta ratio is 2.1 standard deviations above the age-matched average."
Our reports include peer-reviewed citations, z-scores against published normative data, and clear clinical context. Several GPs in the region have received our adult reports and used them to support Right to Choose referrals, NHS adult ADHD pathway access, and shared care arrangements with private psychiatrists.
Yes. Right to Choose allows you to be assessed by a private provider at NHS expense. Having objective brain data in your GP file strengthens the case for referral. The comprehensive package includes a clinical letter specifically designed to support this process. Several clients have had Right to Choose applications accepted after providing our report.
Yes. The clinical interpretation letter contains the objective data and professional language that Access to Work assessors require. Several adult clients have used our letters in ATW applications to secure workplace coaching, assistive technology, or noise-cancelling headphones. We can tailor the letter to focus on workplace impact. See our full Access to Work ADHD guide.
No. This is an objective brain screening. ADHD diagnosis requires comprehensive assessment by a qualified clinician including clinical interview, behavioural history, and assessment of differential diagnoses (anxiety, depression, sleep disorders, thyroid conditions). Our report provides one powerful piece of the puzzle — the neurological data — but diagnosis is your clinician's domain.
A normal TBR doesn't rule out ADHD — it means this specific biomarker isn't elevated. ADHD is complex and not all presentations show elevated TBR. A normal result is still useful data: it helps your clinician narrow the diagnostic picture. It may also provide reassurance if you were uncertain, or redirect investigation toward other possibilities like anxiety, sleep disorders, or burnout.
Yes, in two ways. First, a current scan provides up-to-date brain data that your adult clinician can use. Second, if you're on medication, the comparison scan (£345) shows objective before/after differences — evidence that treatment is working, or data to support a dosage review. Some adult patients also use it to validate a childhood diagnosis they've been questioning.
You can book and pay on someone else's behalf, but the person being screened must attend in person and provide their own informed consent. Many of our adult clients were gently encouraged by partners, friends, or family members who recognised the signs. A gift voucher is also available if you'd like to offer it without pressure.
Macclesfield, Cheshire — easily accessible from Manchester (30 min), Stockport (20 min), Wilmslow (10 min), Knutsford (15 min), Liverpool (1 hr), and the wider North West. Free parking available. We also offer sessions at selected locations by arrangement.
Get objective brain data this week. Same-day report. Evidence that moves you from wondering to knowing.